Healthcare facilities used to be considered “off limits” in times of war. Article 19 of the First Geneva Convention states that hospitals and mobile medical facilities should not be attacked during violent conflict. But last year, there was a 45% increase in attacks on healthcare facilities and medical personnel in countries at war. The remaining medical facilities face power and water cuts even as medical staff, medicine, and surgical supplies dwindle.
Poverty often devastates communities as much as violent conflict does. Venezuela’s economic collapse has driven over 7 million people from their homes, one of the largest displacements of people from a country not at war. Poverty has also decimated Venezuela’s public health care system as doctors and nurses emigrate, medical infrastructure deteriorates, and shortages of medicine, water, and basic health products abound. Patients can’t afford health care, which has caused a swift increase in infant and maternal mortality and infectious disease rates over the last ten years.

In the Venezuelan state of Zulia, a six-month-old Oscar* drinks a bottle of “plantain water,” a mixture of cornstarch, pasta water, and black bean water. Infant formula is too expensive for his mother, Anna*, to buy. “I give the baby bottles of black beans water. When you cook the beans, before they start to get thick, I take the clear water and give it to the baby in the bottle. I know it is not right to give him that, but I do not have formula milk to feed him. It is my way to solve the problem,” she said.
Baby Oscar gets sick because Anna can’t afford to feed him well, take him to a doctor, or buy medicine. Anna is a single mother of five children, who will hopefully eat once a day. On the day we visited, four loaves of bread were on the table, one for each child, and some ham. The math is simple. Anna won’t eat since there isn’t enough bread. This is the daily life of this family. They survive day by day, living in extreme poverty in Venezuela.
“The baby gets sick a lot because I know that I do not feed him well; that depresses me. When I go to the hospital, they do not attend to him well. There are no supplies or medicines. That is what they always tell me. He has lost weight. He gets fever, diarrhea, and when I have to look for medicines, it is a despair for me because they are expensive,” Anna explains.


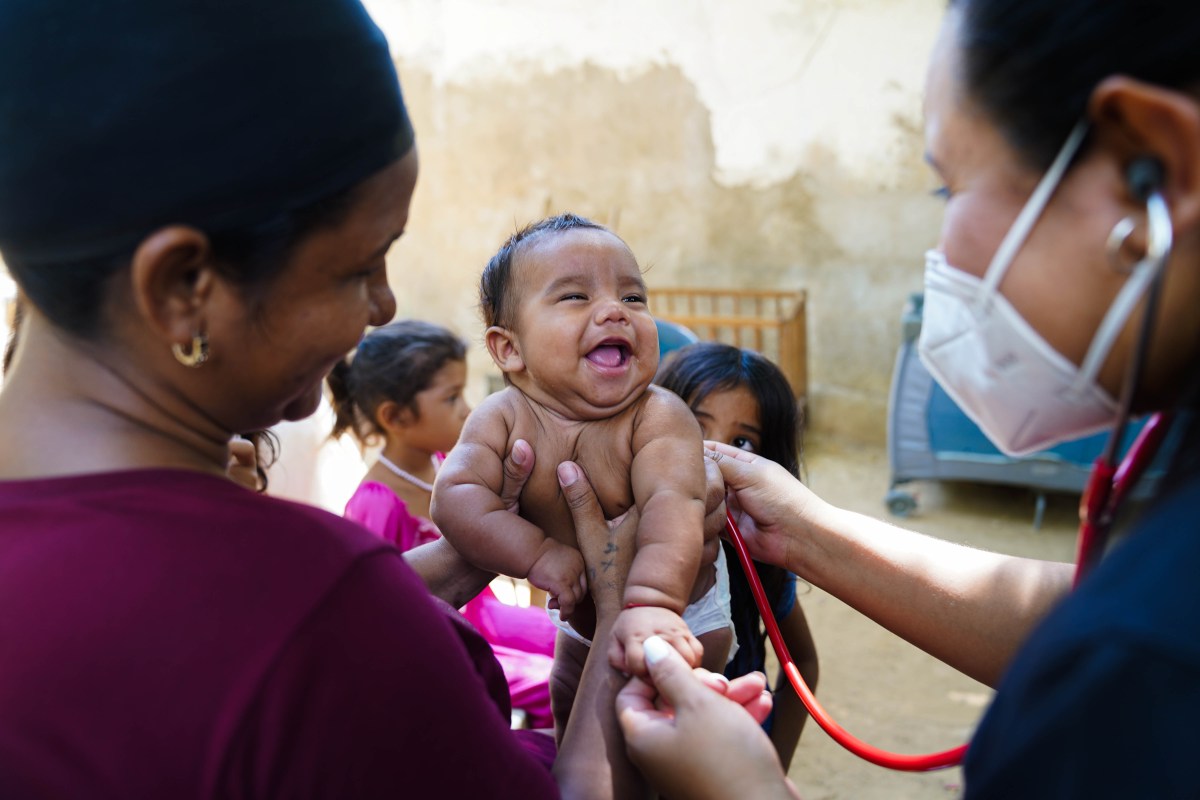
You saw Anna’s need and responded. Thanks to you, our community of peacebuilders brings medical services into six vulnerable communities in Zulia three times a week. Our mobile medical team includes a general practitioner, pediatrician, nurse, general logistics coordinator, and two logistics coordinators to support pharmaceutical needs. Together, this team gives people like Anna and her children medical checkups and medicine, free of charge. Usually, our team sets up their mobile clinic in a local church, but sometimes the team visits people where they are, in their homes. On average, the team serves 70 people each week.
Recently, our team visited Anna, baby Oscar, and Anna’s four older children at Anna’s home. Our mobile medical team examined everyone and provided the medicine they needed. “Thank you for helping my children. The medicines that they give me are a blessing because I could never buy them. Thank you to the doctors and all of you for coming to my humble home. It breaks my heart that people like you care about my children. I am eternally grateful,” said Anna.
Thanks to you, our mobile medical team has served communities in Zulia, Venezuela, for a while. Almost half of our patients are over 50 years old, while 21% are under five, showing that Venezuela’s need for medical services affects the young and old alike. Stay tuned for an update about the medical services you make possible in Venezuela’s Capital District. Your generosity is a reminder that we belong to each other.
*Not their real names
This is part one of a two-part series featuring our medical services in Venezuela.