They drive out of town and keep going, past nameless roads where the street lights end and the paving stops. They navigate roads flooded by autumn rains, past houses and businesses bombed out by ISIS or by liberators—it all looks the same at this point. They finally stop at a small community off the beaten-path, put on their white coats, hang stethoscopes around their necks, and turn, smiling to the first families who venture near.

In 2016, as the Iraqi Army and allied forces pushed north along the Baghdad to Mosul highway, liberating communities from ISIS control, we came behind, in the shadow of the front lines, providing essential care for families fleeing the violence. Two years ago this month we stood with Iraqi doctors and nurses who wanted to practice their skills not only in sterile hospitals, like their colleagues, but also in the places where there was acute need and no access to medical care. We showed up in places like Dream City, an unofficial displacement camp, first with clean water and soon after with a field clinic providing essential and lifesaving care.
Together we continued to partner with Iraqi professionals to provide health services in places where war severely restricted access. In the early months of 2017, we renovated three primary health centers in war-ravaged Mosul, and reopened the first health care center in east Mosul post-war.
In more than a dozen towns impacted by war, together we showed up in the form of primary health centers. These health centers are places not only where babies can be vaccinated, children get stitches, and grandparents get diagnosed with chronic diseases like diabetes and heart disease. These health centers are tangible commitments to devastated communities: ‘You are not alone. We will stand with you in the gap until your community gets on its feet.’
Our commitment allowed countless thousands of displaced Iraqi families to return home and begin rebuilding their lives.


These health centers become hubs for wider community care. Doctors know their patients, and their patient’s needs, well. You provide doctors with a wider range of tools than they learned about in medical school. You provide food packs so that doctors can “prescribe” food when hunger is a roadblock to health. You provide small business grants so that doctors can “prescribe” a small business to vulnerable families who need the opportunity to work and provide for their children.
These doctors work extraordinarily hard to help their communities—crushed by war—to become whole again. And they’re good at it! At some of our health centers, the medical teams saw that, from a medical perspective, their communities are now stable and residents are well cared for.
These medical teams aren’t satisfied with their success, though.
The same spirit that drove them to reopen health centers in devastated communities is driving them out again, into villages dotted throughout the countryside, where no services are reaching—not the government, not other organizations.


Each week, teams from our health centers travel out to surrounding villages where there is currently no health care available. They are meeting families at their point of need with medical treatment, health education, and lots of love.
There are no public buildings here to function as makeshift clinics, no examining tables, no supply rooms with tongue depressors and sterile gowns. But there are lawns with benches. There are living room floors and hard-packed streets.
The teams see the same full range of conditions in the villages they see in their clinics: infectious and chronic diseases including diabetes, ulcers, skin diseases, kidney failure, asthma, hypertension.


At a school for girls, the team found themselves providing care for girls so desperate to stay in school that they were hiding symptoms of serious illness. Without access to medical care, the girls were afraid that their illness would force them to stay home rather than continue their education.
Many girls were diagnosed and provided with prescriptions on the spot—quick relief. Others have been added to lists for follow-up treatment. And every one of them was given the knowledge that they’re no longer alone in their suffering.

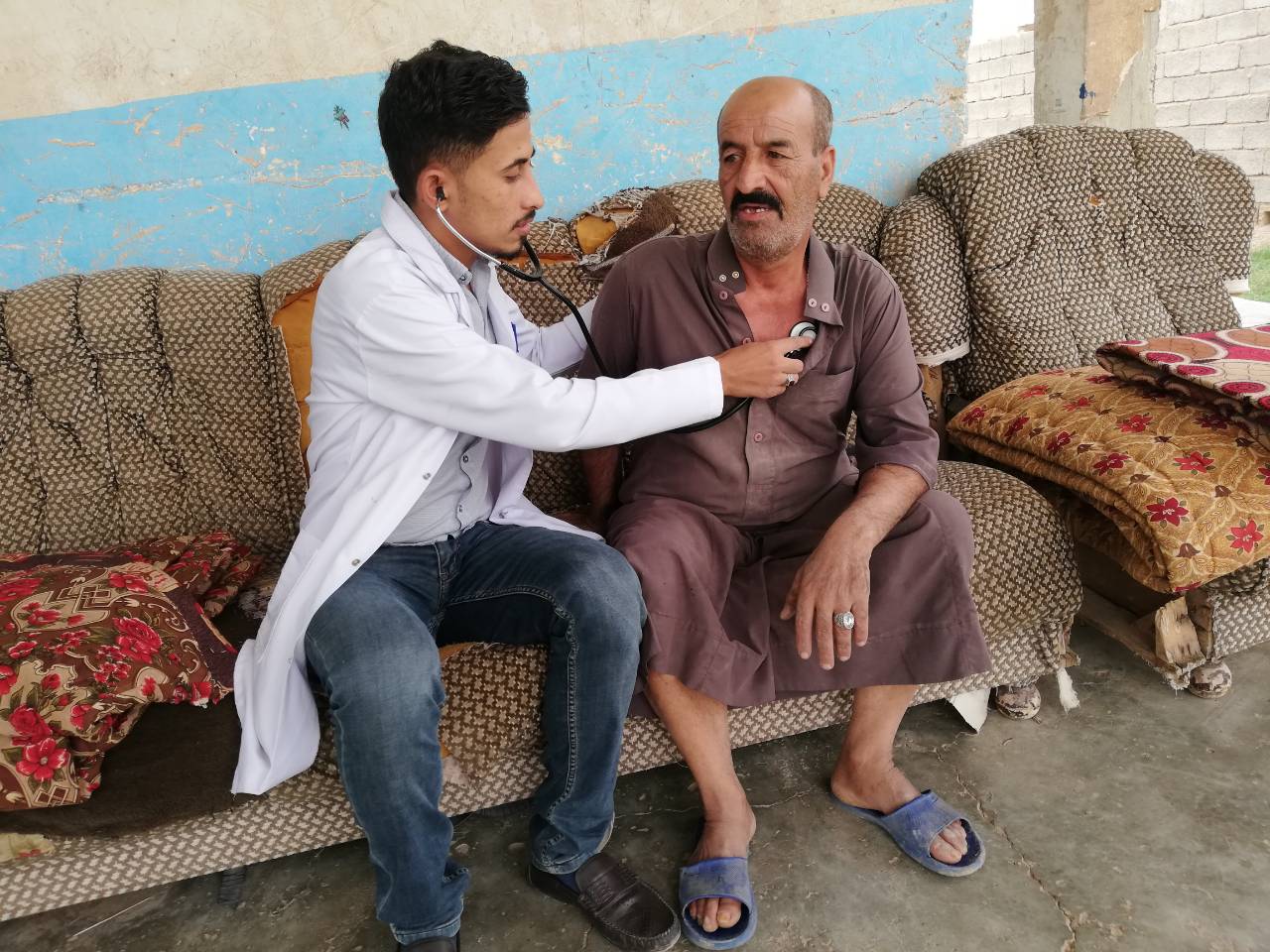

Residents are thrilled by the visits, and frankly so surprised!
This time last year you were providing essential health care through nine primary health centers and mobile clinics. Today, it’s 13 health centers and hospitals, as well as a growing number of remote communities. You may have heard us talk about aspiring to be “first in, last to leave,” and sometimes “first in” looks like sitting on plastic stools at the only crossroad in town, listening deeply to a new mom’s fears. Sometimes it looks like sitting on a living room floor, assessing rashes shared by a whole family. Sometimes “first in” looks like telling a teenage girl with anemia that medication can help and she won’t have to leave school.
There are doctors and nurses in Iraq dissatisfied with the status quo. They are reaching out where others won’t go, meeting patients at their place of need. And you are helping make it happen.


